HWN Jobs
- A REPUTABLE PHARMACEUTICAL COMPANY JOBS
- VICBEE PHARMACY AND STORES (2016) JOBS
- CLINTON HEALTH ACCESS INITIATIVE (1 SLOT) JOBS
- SUBHOL HOSPITAL LIMITED (SHL) JOBS
- ESTEEM DIAGNOSTIC MEDICAL SERVICES LIMITED JOBS
HWN Blogs
- Classical heart healthy foods on HWN BLOGS
- Classical Warning Signs When The Human Liver Begins To Fail on HWN BLOGS
- Myths About Hygiene, Soaps, Germs, Sweat and Smell on HWN BLOGS
- Hernia does not heal on its own on HWN BLOGS
- Classical Essential Oils That Improves Focus Cum Memory on HWN BLOGS
news - Tool to boost diagnosis for bowel cancer in patients under 50 on HWN CANCER back to all News
Tool to boost diagnosis for bowel cancer in patients under 50 on HWN CANCER
GPs have been given access to a new risk assessment tool to help diagnose young people at risk of bowel cancer.
Experts say people under 50 do not act on bowel cancer symptoms quickly enough and 20% have to visit a GP five times before being referred to a specialist.
The new tool will help calculate the risk of the disease based on blood tests, symptoms and a GP's examination.
Bowel Cancer UK told the Victoria Derbyshire programme all GPs should be given access to the "lifesaving" tool.
While 95% of bowel cancer cases occur in people over 50, more than 2,500 people under the age of 50 in the UK are diagnosed with the disease every year - a 45% rise since 2004.
The NHS provides testing for people between 60 and 74 every two years. But experts say when it comes to those under 50, people do not act on their symptoms quickly enough.
Urgent colonoscopy
The new risk assessment tool - which is based on research by University of Exeter and was funded by the Department of Health - calculates the risk of a serious disease as a percentage.
Those found to be at 3% risk or more of bowel cancer should be referred for an urgent colonoscopy, while those between 1% and 3% will be recommended for a faecal calprotectin test, to help diagnose conditions like irritable bowel syndrome (IBS).
Anyone found to be 1% risk or less will require no further tests.
The assessment tool was made available to GPs on the British Journal of General Practice website on Tuesday. Bowel Cancer UK says it now hopes to integrate it into GP practices.
Experts say the new tool is the first of its kind for younger people.
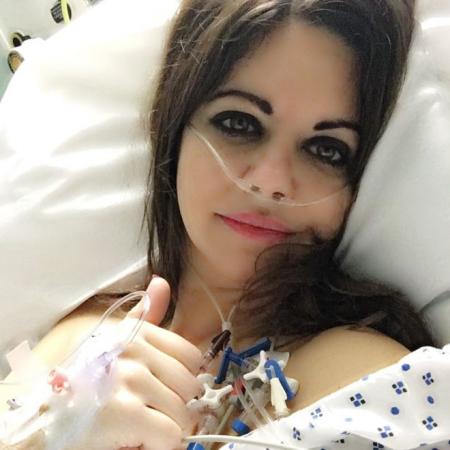
Deborah James, 35, has stage three bowel cancer
Deborah was feeling under the weather for about a year, but blood tests picked up nothing irregular.
However, her symptoms got worse, to the point she was going to the toilet 10 times a day and passing blood "every other day".
After further tests came back as normal she asked for a colonoscopy, which she had shortly before Christmas last year.
She says it was then that everything fell silent in the room. A 6cm tumour was discovered in her rectum.
The first thing I said, was I don't want to die. I screamed at the consultant and I said: I don't want to die, she told the Victoria Derbyshire programme.
I have two beautiful children, and it is mortifying the idea that I might not see them grow up. I was absolutely petrified.
The cancer had spread to eight of her lymph nodes.
I think I am learning to accept the fact that I have limited control over my cancer, she says.
I can eat healthily, I can stand on my head backwards or eat three teaspoons of turmeric a day, I can do what every somebody is suggesting is the latest cancer 'think', but cancer is a very unknown scary thing.
She adds: I have done a lot of crying, I have done a lot of shouting, I have planned my own funeral, I have said thank you, I have said I love you, I have hugged my children and I have laughed with them.
She says she is determined not to spend the next five years wondering which statistic I am going to be, the 60% that is going to be OK, or the 40% that is not.
Second biggest cancer killer
Experts say one problem with diagnosing the under-50s with bowel cancer is that one in four people wait an average of three months before going to see their GP.
It means up to 60% of people under 50 will be diagnosed with Stage 3 or 4 bowel cancer, while fewer than 20% will be diagnosed at the earliest stage of the disease - when survival rates are much higher.
Bowel cancer facts:
It is the UK's second biggest cancer killer
About 16,000 people die of it and a further 41,000 people are diagnosed every year
It is the fourth most common cancer in the UK
If diagnosed early enough, more than 90% of cases can be treated successfully
Five-year survival rates have doubled over the last 40 years
The lifetime risk of men being diagnosed is one in 14, while for women it is one in 19
Deborah Alsina, chief executive of Bowel Cancer UK, said it was vital to diagnose people early "when treatment is likely to be more successful.
She said the new assessment tool "has the potential to help GPs to decide which of their young patients need a referral for further tests and which have less serious bowel conditions.
However, this is just the start, the next step is to ensure that all GPs across the UK have access to this potentially lifesaving tool as part of their day to day practice.
Willie Hamilton, from the University of Exeter Medical School which led the research, added: The tool does not replace clinical judgement but provides more information to base a referral decision.
Source: BBC, HWN AFRICA.
: 2017-03-28 19:03:22 | : 4294
HWN News
- First Polish infant to survive on extreme dialysis on HWN MEDICAL MIRACLES
- Drug resistant tuberculosis end game on HWN INSIGHTS
- Too many women opting for caesarean sections (CS) to give birth on HWN SEX EDU
- The intelligent, strong and fearless Nurse that conquered Ebola on HWN ARCHIVE
- Medhi Benatia, down with injury on HWN SPORTS






